Contact Information
| Telephone: | (852) 2255 4232 |
| Fax: | (852) 2817 2291 |
Background
The Division of Endocrine Surgery (ECS) is the only full-time surgical unit in Hong Kong that solely takes care of patients with a thyroid, parathyroid, adrenal or endocrine pancreatic problem. According to the annual Hospital Authority territory-wide audit (or SOMIP in short), our team has consistently been ranked as one of the highest volume endocrine surgical centers in the territory. Approximately 300 – 350 thyroid resections and 40 – 50 parathyroid resections are done annually by our team of surgeons. Apart from providing the highest standard of surgical care, our team has an immense interest in teaching & learning, research and clinical innovations.
Apart from teaching our own undergraduate medical students, the team has mentored many surgical trainees and overseas fellows interested in ECS. Through this fellowship program, many of our overseas fellows have become a leading surgeon in their respective country.
In research, one of the main focuses has been to gain a clearer understanding of the disease process in benign nodular disease (goiter), thyroid carcinoma, Graves’ disease, hyperparathyroidism, adrenal tumor, pancreatic neuroendocrine tumor and other less common endocrine familial syndromes. The division has been conducting clinically relevant and translational researches. Many of our research work have resulted in high-impact publications and presentations at international conferences allowing a greater dissemination of our experience.
The team has also been innovative in its treatment of various thyroid and endocrine-related diseases. For example, the team was the first in the territory to adapt robotic-assisted thyroidectomy. We were also the first in Asia to use high intensity focused ultrasound (HIFU) ablation in the treatment of symptomatic thyroid nodules. In surgical innovations, we were one of the early adaptors of the trans-oral vestibular thyroidectomy and the first to conduct a registered trial looking the safety of this approach.
Thyroid diseases and thyroid cancer
More than 800 new patients with thyroid diseases are seen and 300-350 thyroid procedures are performed annually. Nodular goiter remains the number one reason (60%) for surgery. Ultrasound-guided fine needle aspiration cytology is commonly done in the outpatient clinic. Our reported incidence of surgical morbidities is among the lowest in the territory. Our permanent hypoparathyroidism and vocal cord palsy are 1.6% and 0.9% respectively.
Thyroid cancer is the most common endocrine malignancy. All patients with thyroid carcinoma are managed by a standard protocol. Adjuvant radioactive iodine treatment and whole body scan, external beam irradiation are given selectively. Patients are closely followed in the Combined Thyroid Clinic jointly with the radiation oncologist.
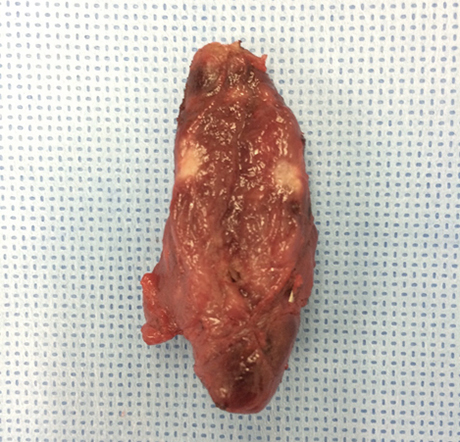
Papillary thyroid carcinoma
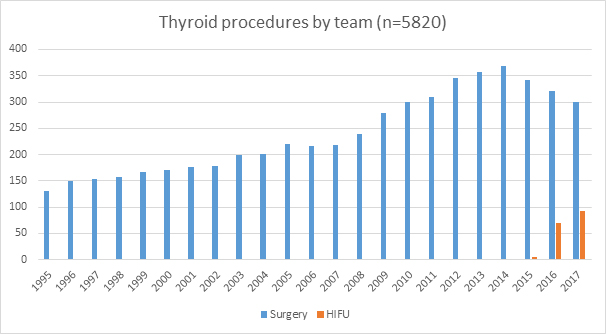
Annual case volume from year 1995 to 2017
Application of HIFU ablation in benign thyroid nodules
HIFU is a form of thermal ablation techniques that has shown to cause significant nodule shrinkage and alleviate nodule-related symptoms.
Ultrasound-guided HIFU device
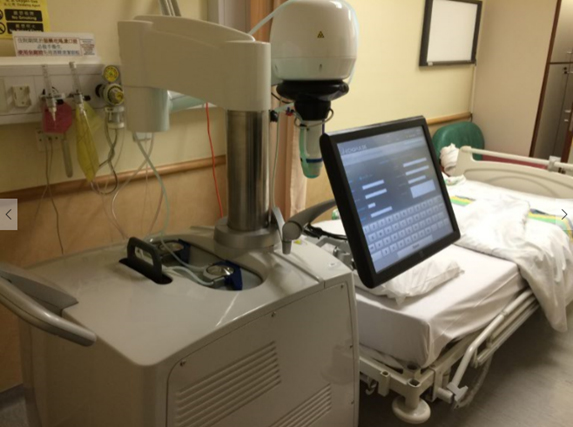
Ultrasound-guided HIFU device
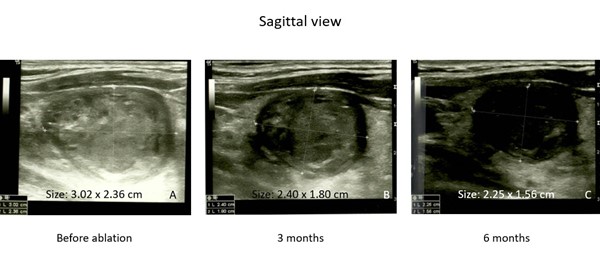
Serial nodule shrinkage after single-session of HIFU ablation
Transoral vestibular thyroidectomy
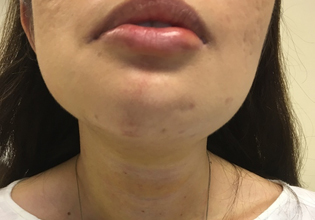
1 week after transoral verstibular thyroidectomy
Parathyroid diseases
Primary hyperparathyroidism (pHPT)
The number of cases of pHPT has been on the rise and surgical resection remains the only option for disease cure. In our experience, over 90% of patients can undergo the minimally invasive approach with biochemical cure confirmed with the intraoperative parathyroid hormone assay.
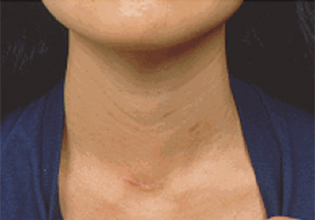
6 weeks after minimal invasive parathyroidectomy
Adrenal diseases
Laparoscopic or minimally approach adrenalectomy
This has been our standard approach in the majority of patients requiring surgery. With this approach, over 95% of patients can be discharged one day after surgery.
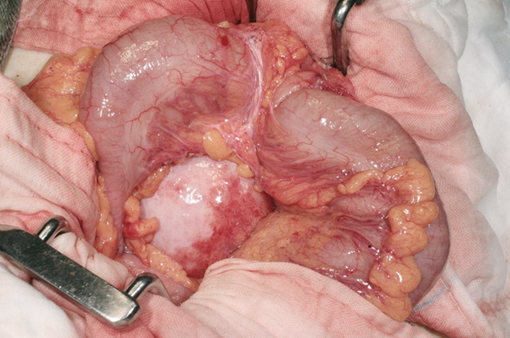
Large invasive adrenal tumor
Pancreatic endocrine diseases
Insulinoma is the most common pancreatic endocrine disease. Preoperative localization studies including CT scan, MRI, endoscopic ultrasound and octreotide scanning are available. Intra-arterial calcium injection with hepatic venous sampling is performed by experienced Radiologists from Department of Radiology with high success rate. For patients with negative localization, a combination of intraoperative localization by palpation and intraoperative ultrasound has achieved a high success rate in surgical treatment of patients with hyperinsulinemia. Minimal invasive surgery by laparoscopic enucleation and distal resection has been performed with success in selected patients.
Recent Publications (reverse chronological)
-
Fung MM, Wong IY, Chan FS, Law TT, Chan KK, Wong CL, Law SY, Lang BH. A Prospective Study Evaluating the Feasibility and Accuracy of Post-operative Laryngeal Ultrasonography (LUSG) in Assessment of Vocal Cord Function After Esophagectomy. World J Surg. 2023 Nov;47(11):2792-2799. doi: 10.1007/s00268-023-07128-9.
-
Perrier N, Lang BH, Farias LCB, Poch LL, Sywak M, Almquist M, Vriens MR, Yeh MW, Shariq O, Duh QY, Yeh R, Vu T, LiVolsi V, Sitges-Serra A. Surgical Aspects of Primary Hyperparathyroidism. J Bone Miner Res. 2022 Nov;37(11):2373-2390. doi: 10.1002/jbmr.4689.
-
Fung MM, Lang BH. Using Intra-Operative Laryngeal Ultrasonography as a Real-Time Tool in Assessing Vocal Cord Function During Radiofrequency Ablation of the Thyroid Gland. World J Surg. 2022 Sep;46(9):2206-2211. doi: 10.1007/s00268-022-06596-9.
-
Fung MM, Lang BH. Efficacy of single-session radiofrequency ablation (RFA) in rendering euthyroidism for persistent/relapsed Graves' disease, a pilot study. Eur Radiol. 2023 Sep;33(9):6534-6544. doi: 10.1007/s00330-023-09620-1.
-
Fung MM, Tam DS, Lui DT, Lang BH. Pre-operative Cinacalcet Administration Reduces Immediate Post-operative Hypocalcemia Following Total Parathyroidectomy in Severe Renal Hyperparathyroidism. World J Surg. 2023 Aug;47(8):1986-1994. doi: 10.1007/s00268-023-07030-4.
-
Chen DW, Lang BH, McLeod DSA, Newbold K, Haymart MR. Thyroid Cancer. Lancet. 2023 May 6;401(10387):1531-1544. doi: 10.1016/S0140-6736(23)00020-X.
-
Fung MM, Lang BH. Intraoperative trans-laryngeal ultrasound (LUSG) of the vocal cord is a novel method of confirming the recurrent laryngeal nerve (RLN) integrity during thyroid and neck surgery. Surgery. 2022 Jan;171(1):165-171. doi: 10.1016/j.surg.2021.05.062.
To check out our latest publications, please follow the below link:
https://www.ncbi.nlm.nih.gov/pubmed/?term=lang+bhEndocrine Surgery
Division Chief
Professor Matrix Man-Him FUNG馮文謙
Clinical Assistant Professor
- MBBS(HK), FRCS, FCSHK, FHKAM(Surgery)
| (852) 2255 4232 | |
| mmhfung@hku.hk | |
| HKU Scholar Hub |
Staff List
| Name | Title | Position | Staff types | Telephone | |
|---|---|---|---|---|---|
| Professor Brian Hung-Hin LANG 梁熊顯 |
Division member | Clinical Professor (Part-time) | Academic staff | (852) 2255 4232 | surgery@hku.hk |
| Dr. Yan LUK 陸恩 |
Division member | Resident (Specialist) / Honorary Clinical Tutor | Hospital Authority staff | (852) 2255 4232 | surgery@hku.hk |














